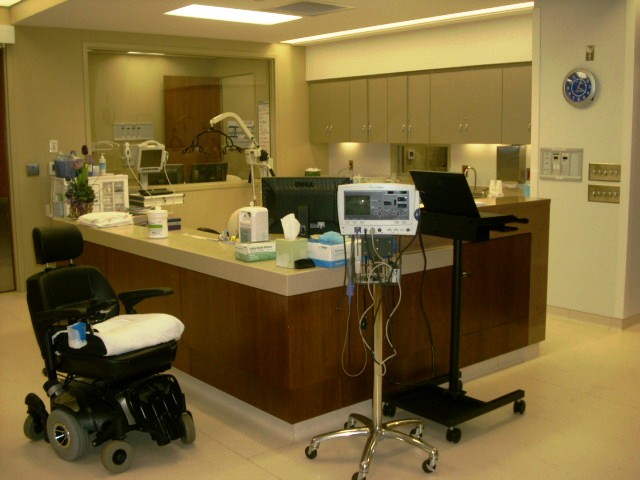
Raleigh Access Center
 North Carolina Nephrology is pleased to provide modern hemodialysis vascular access care in a state-of-the-art outpatient facility. The access center is designed to provide timely procedural interventions on dialysis access in a convenient and comfortable setting. The facility is located on the first floor of Wake Plaza across the street from Wake Med Hospital on New Bern Ave in Raleigh, NC. Jeff Hoggard MD, our medical director, is credentialed in interventional nephrology procedures, is a board certified nephrologist, and has performed over 9000 interventional procedures.
North Carolina Nephrology is pleased to provide modern hemodialysis vascular access care in a state-of-the-art outpatient facility. The access center is designed to provide timely procedural interventions on dialysis access in a convenient and comfortable setting. The facility is located on the first floor of Wake Plaza across the street from Wake Med Hospital on New Bern Ave in Raleigh, NC. Jeff Hoggard MD, our medical director, is credentialed in interventional nephrology procedures, is a board certified nephrologist, and has performed over 9000 interventional procedures.
Hemodialysis vascular access has been described as the “lifeline” of the dialysis patient. At the Raleigh Access Center our goal is to help create and protect this lifeline. This expert care is provided according to national guidelines and standards and is more expeditious and less costly than access care at the hospital.
Procedures performed at Raleigh Access Center
1. Declot or Thrombectomy – This procedure removes the clot and re-establishes blood flow in the dialysis access. A clotted dialysis access cannot be used for hemodialysis until the access is declotted, and therefore, we aim to perform this procedure as soon as the clotted access is discovered.
2. Angiogram/Fistulogram – A contrast agent is injected through the graft or fistula to determine the cause of the blood flow problem. When a stenosis or narrowing is found, this procedure may also require an angioplasty and/or a stent.
3. Angioplasty – A balloon catheter is inserted into the graft or fistula and inflated to dilate a stenosis or narrowing.
4. Stent Placement – This involves placement of a metallic stent typically to help hold open a blood vessel that continues to narrow after an angioplasty.
5. Tunneled Dialysis Catheter Insertion – A dialysis catheter is placed in one of the central veins in the neck or leg.
6. Tunneled Dialysis Catheter Exchange – Replacement of a catheter for a new or different type of catheter.
7. Tunneled Dialysis Catheter Removal – Removal of catheter when no longer needed.
8. Temporary Catheter Insertion – This dialysis catheter is usually placed in a central vein and is intended for less than one week of useage
9. Vessel Mapping – Before surgery to create an arteriovenous access, vessel mapping uses ultrasound and venography to determine the artery and vein anatomy to best determine what type of access surgery should be done and where that access should be created.
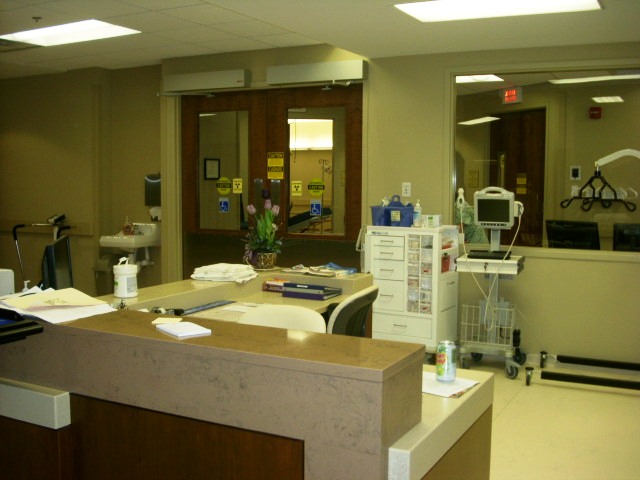
Common Reasons For Referral to the Access Center.
1. Currently have a dialysis catheter and need to have vessel mapping prior to surgery to place an arteriovenous access in the arm.
2. Difficulty cannulating the access
3. Arm swelling
4. Increased venous pressures on the dialysis machine
5. Increased negative arterial pressure on the dialysis machine
6. Yellow light on the stop light ( not green) during dialysis
7. Low Kt/v or URR which means poor clearances on dialysis
8. Pain in the access arm or hand
9. Prolonged bleeding at the needle cannulation sites
10. Dialysis catheter not achieving blood flow of at least 300 ml/min
11. Dialysis catheter infection
12. Low access flow measurement (on the dialysis machine or transonic device) indicating an arteriovenous graft with access flow less than 600 ml/min
13. Low access flow measurement ( on the dialysis machine or transonic device) indicating an arteriovenous fistula with access flows less than 500 ml/min
Procedure Instructions
Your dialysis center or a staff member at one of our facilities will be able to assist you with specific instruction regarding preparation for your procedure.
1. In general there are no restrictions about taking medications prior to these procedures except for blood thinners or anti-platelet medications. Check with your Nephrologist to be sure it is safe for you to hold these medications and he/she may have specific instructions regarding other medications.
2. Notify our center prior to the procedure if you have an allergy to latex and/or contrast (dye).
3. Moderate intravenous sedation (“Conscious sedation”) is used for many of our procedures to ensure patient comfort. A local anesthetic is also used as well.
4. One should not consume food for 8 hours prior to receiving moderate sedation. It is very important for someone to drive you home after receiving sedation as you should not drive for 24 hours after the procedure.
5. These specific written instructions will be given to you and reviewed with you by your dialysis center staff. These instructions will also be reviewed with you by phone from the access center.
Our Outcomes
There is strong evidence that early intervention to treat vascular access problems can reduce major complications. We believe it is important to:
• Provide timely and cost effective treatment of the ESRD patient.
• Minimize hospitalization related to access care for the ESRD patient.
• Provide a patient report to your doctor and dialysis facility in a timely manner.
• Provide patient education regarding access care.